By Jasmin Joseph, Yes! Magazine
For Black and Indigenous communities, it takes more than therapy and medication to tackle mental illness – a holistic approach is essential
The ways of our ancestors are buried deep in our consciousness, emerging unwittingly and at random. We see our elders perform them in subversive ways, such as grandmothers entering a meditative state in the middle of the day by “resting their eyes” or expressing that a child has “been here before”— a tacit recognition of reincarnation and acknowledgement of the inherent sanctity of the very young and very old. I don’t think it’s a coincidence that the West African goddess of fertility, Yemanjá, is also the goddess of fishermen. To this day, dreaming of a fish in Black American families is an omen of pregnancy.
If these positive cultural markers are passed down, it follows that the negative ones are as well. My own mental health journey began after my OB-GYN suggested that I seek psychiatric treatment. While checking my vitals, he was alarmed by my spiking diastolic pressure as I prepared to tell him the reason for my visit. I informed him distractedly that this “just happened” to me when I got nervous. His brow furrowed in concern as he asked me if I’d ever talked to someone about this. I nearly laughed. “About what?”
Until then, I had never before considered psychiatric care. During college, I only vaguely remember learning about counseling services, and certainly never considered utilizing them. To me, mental “illness” was recognized only in its most extreme forms—severe bipolar or major depressive disorder, psychosis, delusions, schizophrenia—and therapy reserved for the truly “crazy.” It turns out, I wasn’t alone in this belief.
Mental health within cultural context
The difficulty of seeking and affording culturally competent mental health treatment in the U.S.— one of few developed nations without a universal health care system — is compounded by social stigmas within Black and Indigenous communities. This can be traced back to not only a deep skepticism of Western medicine, but also to pervasive cultural beliefs that admission of mental illness is a sign of weakness.
My journey included the destigmatization of mental illness and transformed into an acceptance of mental healthcare as an inextricable part of holistic wellness. When I discovered that the origins of many individual issues can be traced to familial and generational harms, it became apparent that the closer intervention and treatments are to our ancestral ways, the more effective they can be.
There have long been major blind spots in conventional Western approaches to treating mental illness in African American and Native American communities. Centuries of living under the psychological stresses of slavery, Jim Crow segregation, settler colonialism and genocide are bound to impact cognitive functioning and manifest in what we now term “mental illness.”
My first step was to find a therapist to whom I could relate. Suspicious of psychiatrists, whom I saw as the health system’s high-end dope dealers, but still recognizing that I needed help, I did a simple internet search for “Black women therapists near me.” I found a website called Therapy for Black Girls, created by Dr. Joy Harden Bradford, and decided to begin with no-frills talk therapy through a provider on the website’s directory. Even though I was still in the infancy of my wellness journey, I knew I was beginning a process of deep excavation into the fibers of my life and, by extension, the lives of my parents, their parents and their parents’ parents.

As a school psychologist working in college counseling centers, Dr. Joy, as she prefers to be called, noticed that Black women were not using her services at the same rates as their non-Black peers. This inspired her to begin Therapy for Black Girls, an online media network and therapy directory that includes more than 1,400 Black women therapists and other therapists of color around the nation.
Dr. Joy notes, “Symptoms of mental health concerns can look different in Black women, and without clinicians who are culturally attuned to our community, important information can be missed.” In my own family, while there were few cases of diagnosed mental illness, there were ample “short tempers,” “weak constitutions” and “bad nerves.” Although no one would call them as such, there were phobias too: of driving, flying, fireworks, big crowds and enclosed spaces.
How trauma is passed
The Diagnostic and Statistical Manual of Mental Disorders (DSM-5) does not include “intergenerational trauma” in its classification of diagnoses used by mental health professionals, but the most recent edition expands its definition of trauma to include the effects of direct and indirect exposure.
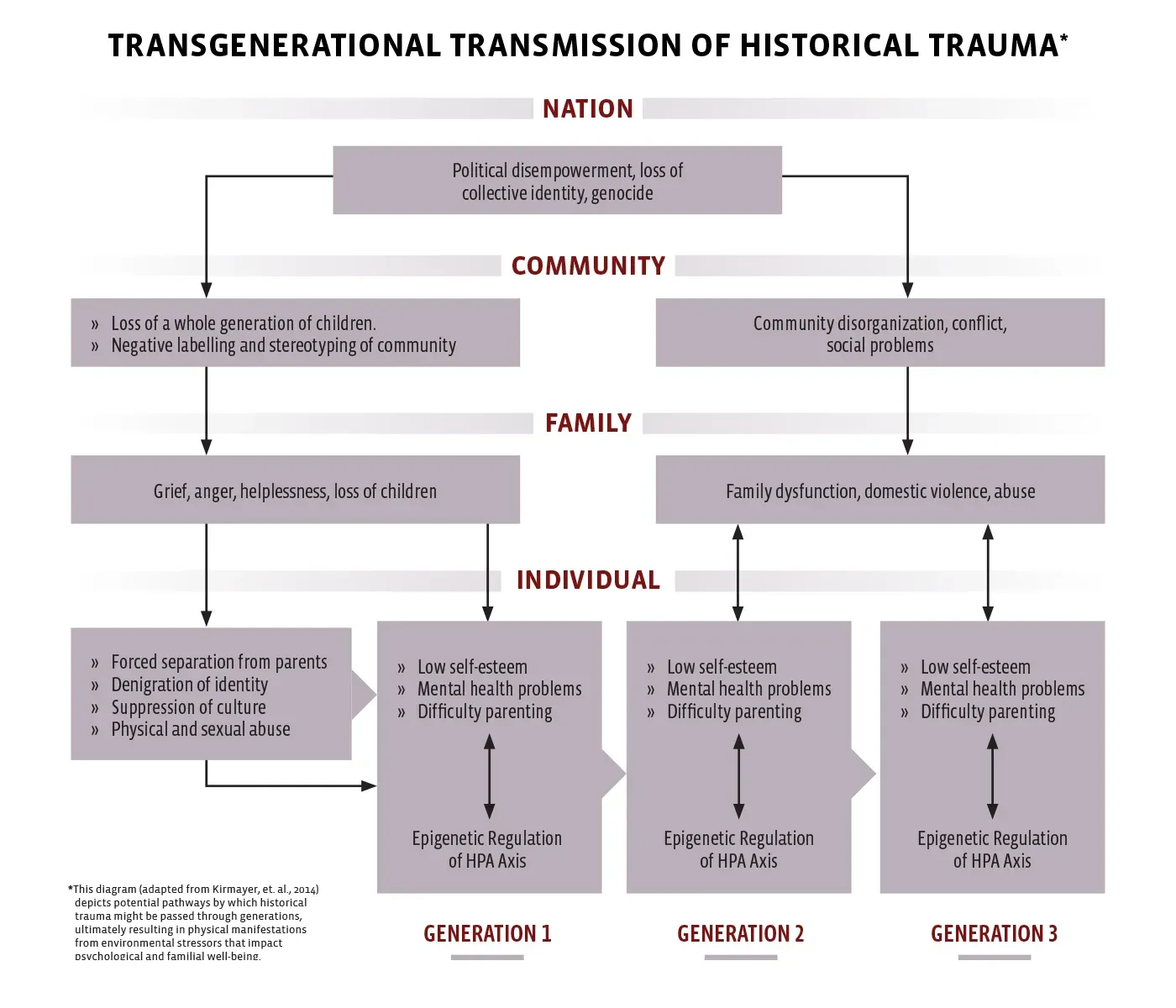
Despite its lack of a “formal” classification, the concept of intergenerational trauma is widely accepted by psychologists and historians alike. It was first identified in the 1960s among the children of Holocaust survivors and has since been applied to Indigenous groups of the Americas and Australia as well as victims of genocide or ethnic cleansing, such as Armenians in Turkey. The term “historical trauma” was coined by Dr. Maria Yellow Horse Brave Heart in the 1980s in relation to the colonization, forced relocation and assimilation of Native Americans.
In 2014, psychologists William Hartmann and Joseph Gone published a paper based on interviews with two influential Native American medicine men from a Great Plains reservation. They recognized in the men’s teachings their unique definition of historical trauma summarized by four C’s: Colonial Injury, Collective Experience, Cumulative Effects and Cross-Generational Impacts.
Up until as recently as the late 2010s, there was little study of the impact of historical and intergenerational trauma on African Americans. The little that does exist often begins with slavery and continues through the legacy of racial discrimination as something separate from the historical trauma of the people native to the Americas. However, when we also view Africans of the diaspora as forcibly displaced Indigenous people, the applicability of the medicine men’s framework to the experience of African Americans is apparent as per Hartmann and Gone’s call for a “spiritual perspective” on the need for healing and the necessity of large-scale, “socio-structural” change.
Similar ideas are becoming more commonplace. For example, the perspectives of Ehime Ora, a holistic wellness educator and author of Ancestors Said: 365 Meditations for a Peaceful Year, and Allie Dyer, co-founder of youth organization Brown Girl Rise and a medical student at the Oregon Health & Science University School of Medicine, echo the aforementioned ideas of the medicine men.
A holistic approach to Black and Indigenous mental health
As an African spiritualist, Ora notes one of the main differences between traditional Indigenous and Western approaches to healing is that in the former, “the presence of spirit is never ignored in the diagnostics of an individual’s health or well-being.… The mind, body, and spirit are never separated — [they] deeply rely on one another for true, balanced health and holistic wellness.”
Dyer, who began Brown Girl Rise with a group of other Oregon-based organizers, advocates for socio-structural changes to medicine in the same way that we demand systematic change for structural violences. She believes the medical community needs to “radically reformulate the theoretical paradigms within allopathic medicine to reflect the reality of our patients and the communities they are part of.”
Growing up, Dyer saw firsthand the minimal access and education Black and Indigenous youth had about their health and bodies. As a medical student, she noted that important social and political contexts were left out of medical teachings. Today, Brown Girl Rise has created community and provided health education that includes historical contexts of coercion and violence. In this way, she says, “a small biology lesson is also a political one,” empowering Brown Girl Rise participants to make their own decisions about their bodies and health.
According to Dyer, who also holds a master’s degree in public health from the Harvard University School of Medicine, this context becomes especially important when we recognize the cumulative impact of historical trauma in both Black and Indigenous communities. It can present in myriad ways, including but not limited to dissociation, emotional numbing, apathy, substance abuse, domestic violence, depression and suicide. Without a holistic understanding of traumatic experiences in Black and Indigenous communities, a purely physical or psychological approach to treating mental health issues may be misguided.
Making community wellness integral to mental health
After more than three years of cognitive behavioral and art therapy, I continued to struggle with troubling physical symptoms— racing heartbeat, digestive issues and dizzying panic attacks. Again, I was advised to consult a psychiatrist. My diagnosis was a pairing not unusual for a young woman my age: generalized anxiety disorder coupled with obsessive-compulsive disorder, defined by intrusive and “ego-dystonic thoughts.” At the recommendation of my therapist and a new psychiatrist, I began taking a low dosage of antidepressants. I put off filling the prescription for a few weeks and waited a few more to start taking the medication, considering it somehow “cheating” to seek outside assistance for my wellness journey — the same sentiment that fueled my initial resistance to therapy.
The belief that we must heal alone is what Ora calls one of the most harmful teachings of Western approaches to wellness. Understanding the generational impacts of trauma helped me become more empathetic with myself and others like me. I began to view mental illness less as a series of disorders and more as a response to our environments. This lessened the stigma I felt in seeking comprehensive treatment to manage it. It worked. After beginning a small dosage of antidepressants, my physical symptoms dramatically reduced and the intrusive thoughts stopped completely.
Indigenous care and healing practices are not only communal, but interdisciplinary. As Ora explains, “From the priest who will diagnose your spiritual health to the herbalist who will provide you with remedies, there are multitudes of individuals having a hand in your healing process.” In this way, our wellness as individuals is inextricable from the wellness of the whole community.
From this new perspective, it finally made sense for me to tackle mental health not only psychologically (via therapy), but also biologically (in my brain) and, ultimately, structurally (in the workplace, the food system, the economy and so on). Our healing should not be conducted in isolation nor rely on a single solution or individual. When we approach healing in this way, there are ripple effects. Dr. Joy summarizes it best: “When we take steps to heal, we give others the courage to do the same.”
Read the original article here.
Jasmin Joseph is a writer and researcher from Yonkers, New York. Her work in Teen Vogue, The Republic Journal, ZORA and other publications details the full breadth of her experience as a Black American woman of African, Native American and European descent. She is currently a staff member at the Producers Guild of America.


